Hi everyone!
My name is Maryam Almotawaa, and I’m a 4th-year pharmacy student.
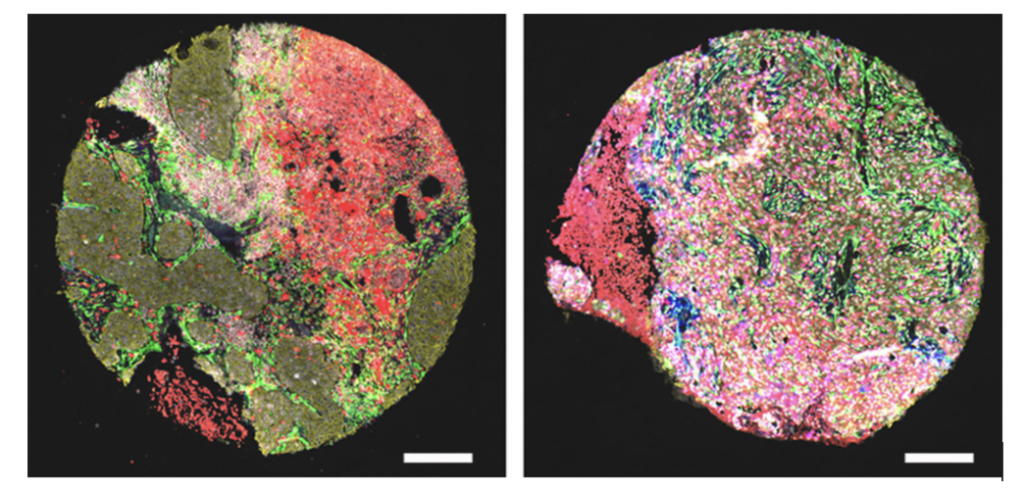
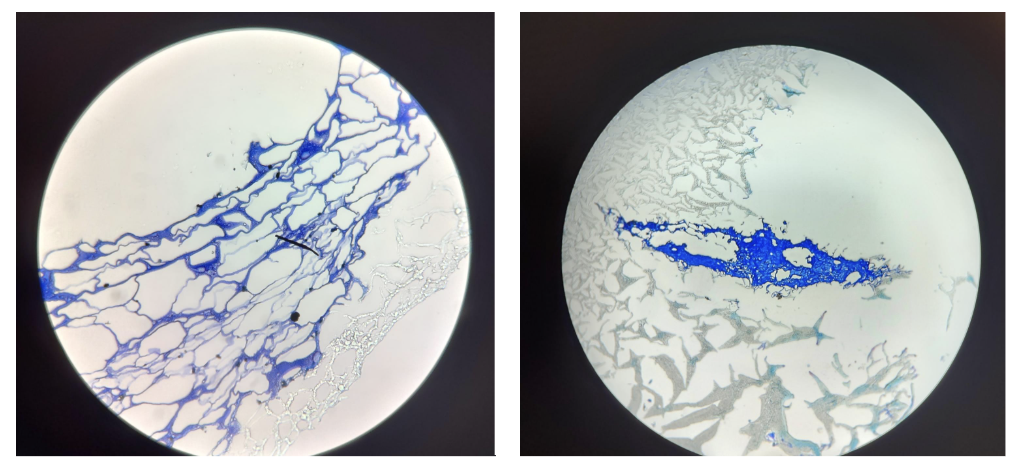
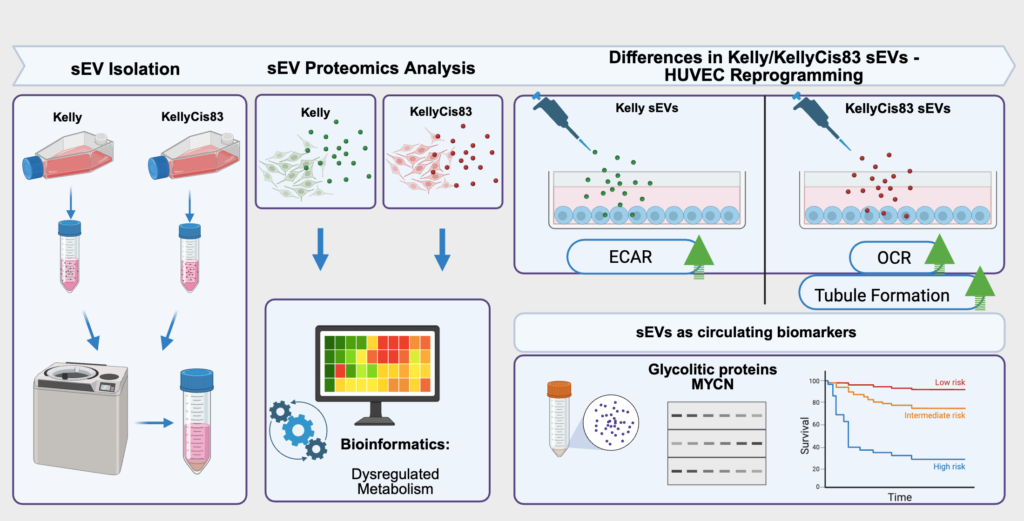
I am working on research to identify a promising tumour-associated antigen for immunotherapy. I used the R2 platform to review datasets, including neuroblastoma and non-small cell lung cancer. I spent some time in the lab observing Lin and Eve working on a Western blot for GPC2, a promising neuroblastoma and non-small cell lung cancer antigen. I was involved in a small part of a Western blot experiment in which I washed the secondary antibody. Even though it wasn’t a big task, it made me realise that even small steps matter and can affect the final result.
Outside my academic life, I really enjoy spending quality time with my friends, whether that’s catching up over coffee or exploring new food spots around Dublin. I also value having time to unwind and recharge, especially after busy academic periods, as it helps me maintain a good balance between my studies and personal life.
Written by Maryam Almotawaa